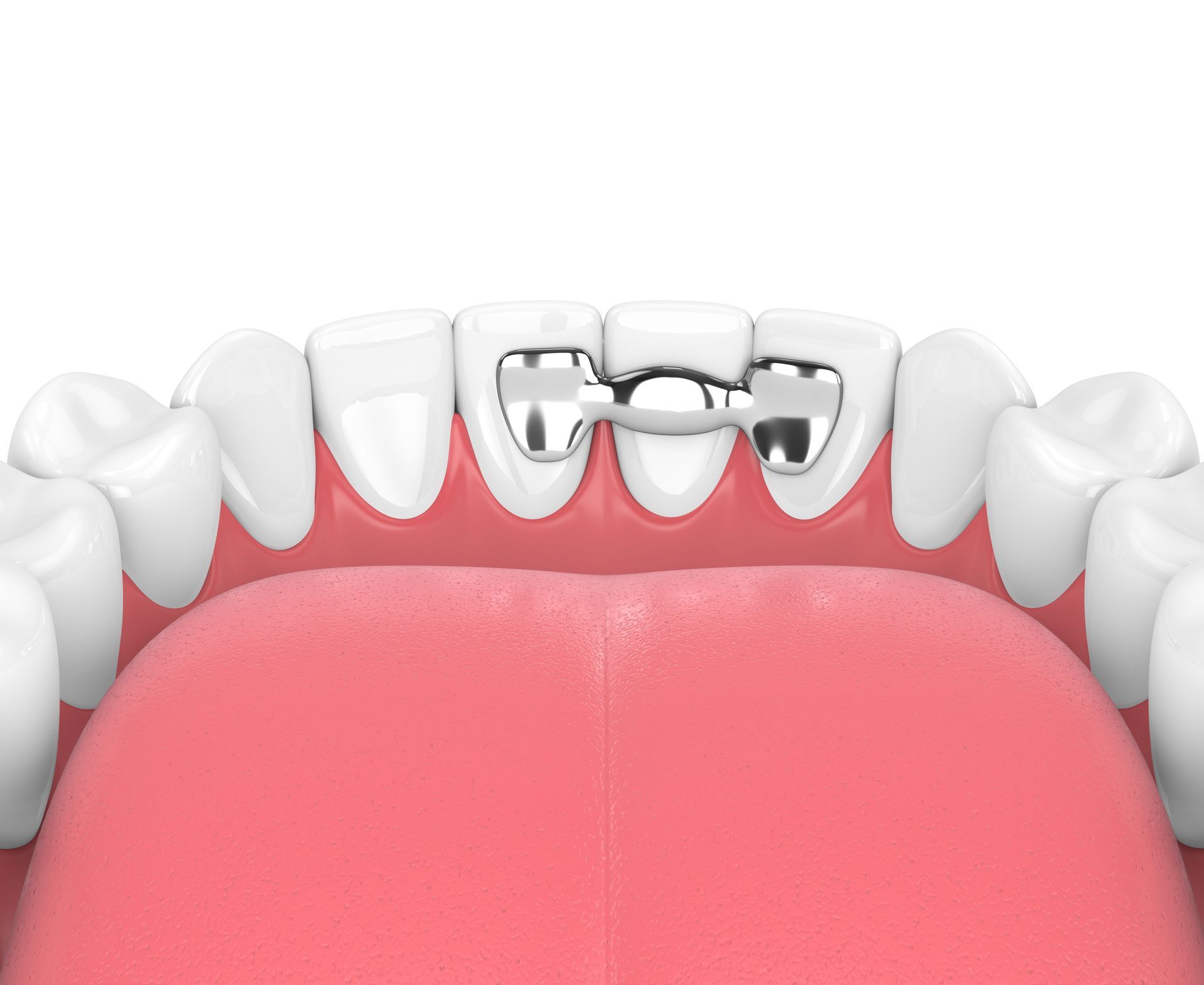
DENTIST IN BOISE, ID YOU CAN TRUST
At Atlantis Dental Care, we're committed to providing world-class general, restorative, and cosmetic dental care in Boise, ID for each and every patient.
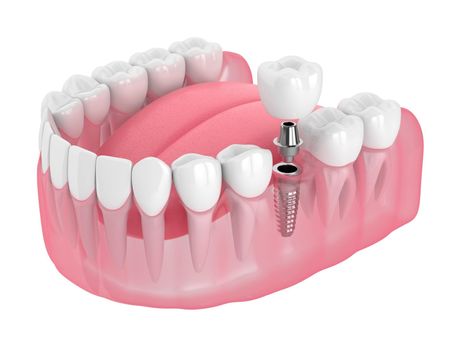
Single Tooth Dental Implants
Starting at
$3,200
Includes Dental Implant, Premium Custom Abutment, and Crown
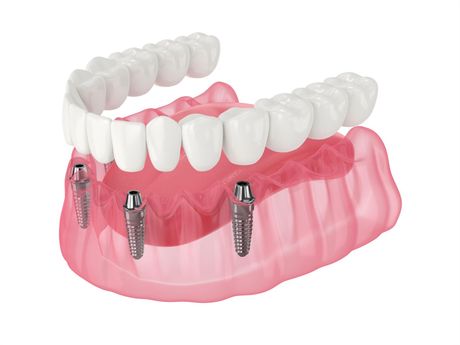
All-on-4 Dental Implants
Starting at
$16,500
Includes All Extractions, Implants and Bone Grafting, and Final Porcelain Teeth
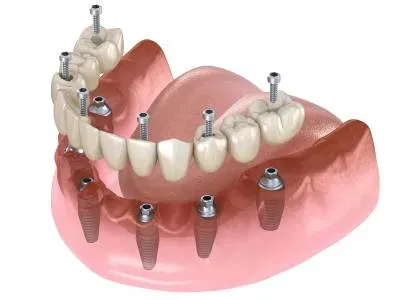
All-on-6 Dental Implants
Starting at
$18,500
Includes All Extractions, Implants and Bone Grafting, and Final Porcelain Teeth
EXCEPTIONAL DENTAL CARE IN Boise, ID
putting patients first
There are many dental offices for your family to choose from, but how do you know who will go above and beyond? At Atlantis Dental Care, we've taken every step we can to make our patients comfortable from the moment they step through our doors. From a friendly greeting at the front desk and complimentary waiting room amenities to a television at each treatment chair, you'll feel right at home. You will receive compassionate treatment from each member of our caring and knowledgeable team so that you can leave happy, with a healthy smile.
Dr. David Cantwell, DDS talks about how to choose the right dentist
Meet David L. Cantwell, DDS, FAGD, Diplomate ABOI
TOp-Rated dentist in boise, id
Dr. David L. Cantwell is extremely passionate about helping patients to achieve the functional, beautiful smiles they deserve. Whether it's a routine exam or addressing an issue that a patient has been struggling with, he aims to provide reliable, affordable dental care. Never satisfied with the status quo, Dr. Cantwell works to continually increase his expertise in dentistry and incorporate the latest in dental technology into the practice.
Our Dental Services
Whether you're looking to maintain your dental health, straighten your smile, restore the function of your teeth, or address a dental emergency, the team at Atlantis Dental Care delivers. Explore our many different services and learn more about which treatments are available to you!
Recent Smile MakEovers
Are you looking for a more even, whiter, flawless smile? We can create a custom treatment plan to address your exact needs and goals, resulting in a totally unique smile makeover. Take a look at some recent transformations we have helped patients with!
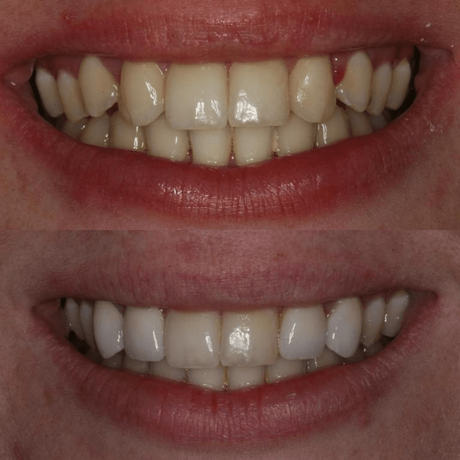
Using Veneers to Give a More Even Smile
Veneers can help provide uniformity to the color and shape of the teeth, resulting in a more even smile that you'll be proud to show off to family, friends, and strangers!
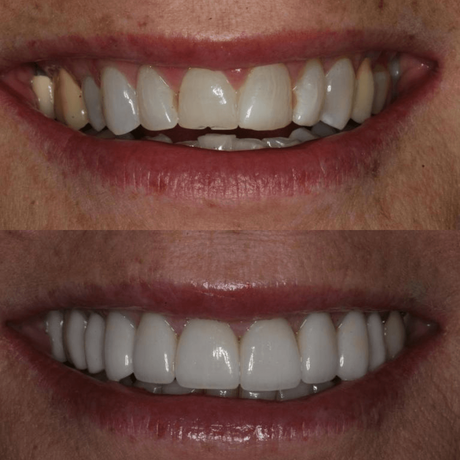
Full Mouth Makeover Gives a Perfect Smile
Whether your teeth are plagued by chips, cracks, decay, or discoloration, we have the treatment options to provide a fully restored, beautiful, and properly functioning smile.
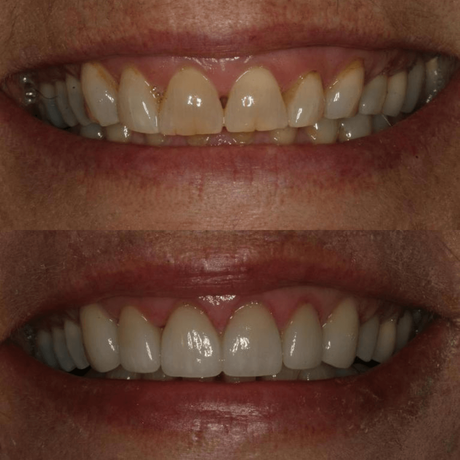
Correcting Smile Worn Down by Grinding
Many patients struggle with teeth grinding (bruxism) and the negative effects that accompany it. Luckily, there are options to restore the appearance of your teeth!
Payment Options We offer
We understand that for some patients, the cost of dental care can prevent them from seeking treatment. It's our mission to ensure we provide the resources and options necessary for everyone in the Boise area to get the dental care they deserve.
All Major Credit Card Companies
When it comes to paying for care, we aim to make it as easy as possible by accepting all major credit cards as well as cash and debit cards.
We Accept All PPO Insurance Plans
Atlantis Dental Care accepts all PPO insurance plans, so you don't need to worry whether we'll be able to work with your insurance provider.
Financing Plans Available
We can connect you with several different options for financing to break your cost of care down into more affordable, easy payments.
In-Office Dental Loyalty Plan
Our in-office loyalty plan is a great option for those who may not have dental insurance and want to save on preventative care and other treatments.
What Our IDAHO Patients Say
Nothing speaks volumes about our service more than the feedback of our patients! Check out what is being said online about our care:

Overall Rating 4.8
Read Our Blog